Sunday Poster Session
Category: Stomach
P1389 - Gastric and Duodenal Pseudomelanosis: A Rare Association with Chronic Iron and Diuretic Therapy
Sunday, October 22, 2023
3:30 PM - 7:00 PM PT
Location: Exhibit Hall
- MS
Muhammad Usman Shahbaz, MBBS
Allama Iqbal Medical College
Orlando, Florida
Presenting Author(s)
Muhammad Usman Shahbaz, MBBS1, Qasim Manzoor Amjad, MBBS1, Bilal Khan, MBBS1, Mariyam Qureshi, MBBS2, Muhammad Shariq Akram, MBBS2, Khalil Ur Rehman, MBBS2
1Allama Iqbal Medical College, Orlando, FL; 2King Edward Medical College, Orlando, FL
Introduction: Upper GI pseudomelanosis is a rare, benign condition of unknown etiology and unrevealed significance. It presents endoscopically as speckled black pigmentation of the mucosa and histologically as dark inclusions within macrophages of the lamina propria. To date, around 10 cases of the combined occurrence of gastric and duodenal pseudomelanosis have been reported. We present a case of concurrent gastric and duodenal pseudomelanosis incidentally diagnosed on upper GI endoscopy.
Case Description/Methods: A 59 year-old-female with a medical history of esophageal stricture, non-ischemic cardiomyopathy, and iron deficiency anemia being treated with furosemide and oral iron supplementation was hospitalized for an acute episode of diverticulitis. After her condition improved, she developed non-bloody emesis. Upper GI endoscopy was performed to investigate the possibility of esophageal stricture. Endoscopy demonstrated dark pigmentation of the entire gastric mucosa with mild diffuse involvement of the duodenum. Cold forceps biopsies were taken at the pre-pyloric area of the stomach and the duodenum for the histopathological examination of the lesions. The biopsy specimen revealed pigment-laden macrophages in the lamina propria, confirming the combined presentation of gastric and duodenal pseudomelanosis.
Discussion: Upper GI pseudomelanosis has been linked to various comorbidities, including upper GI bleeding, chronic renal disease, hypertension, and medications such as oral iron, furosemide, hydrochlorothiazide, propranolol, and hydralazine. The present case shows a similar association with iron and furosemide but without the presence of chronic kidney disease, in contrast to all the previously reported cases that suggest a very strong association with iron therapy or chronic renal failure with pseudomelanosis. In addition, women have been reported to have the most cases compared to men. It has been postulated that drug-based sources of sulfur, such as furosemide, disrupt iron transport and cause iron accumulation within macrophages. While the pathogenesis is not clearly understood, no clinical or prognostic significance has been described and no surveillance or follow-up guidelines have been identified. Therefore, it is essential to diagnose patients early on histopathology findings and to avoid unnecessary testing and interventions.
Disclosures:
Muhammad Usman Shahbaz, MBBS1, Qasim Manzoor Amjad, MBBS1, Bilal Khan, MBBS1, Mariyam Qureshi, MBBS2, Muhammad Shariq Akram, MBBS2, Khalil Ur Rehman, MBBS2. P1389 - Gastric and Duodenal Pseudomelanosis: A Rare Association with Chronic Iron and Diuretic Therapy, ACG 2023 Annual Scientific Meeting Abstracts. Vancouver, BC, Canada: American College of Gastroenterology.
1Allama Iqbal Medical College, Orlando, FL; 2King Edward Medical College, Orlando, FL
Introduction: Upper GI pseudomelanosis is a rare, benign condition of unknown etiology and unrevealed significance. It presents endoscopically as speckled black pigmentation of the mucosa and histologically as dark inclusions within macrophages of the lamina propria. To date, around 10 cases of the combined occurrence of gastric and duodenal pseudomelanosis have been reported. We present a case of concurrent gastric and duodenal pseudomelanosis incidentally diagnosed on upper GI endoscopy.
Case Description/Methods: A 59 year-old-female with a medical history of esophageal stricture, non-ischemic cardiomyopathy, and iron deficiency anemia being treated with furosemide and oral iron supplementation was hospitalized for an acute episode of diverticulitis. After her condition improved, she developed non-bloody emesis. Upper GI endoscopy was performed to investigate the possibility of esophageal stricture. Endoscopy demonstrated dark pigmentation of the entire gastric mucosa with mild diffuse involvement of the duodenum. Cold forceps biopsies were taken at the pre-pyloric area of the stomach and the duodenum for the histopathological examination of the lesions. The biopsy specimen revealed pigment-laden macrophages in the lamina propria, confirming the combined presentation of gastric and duodenal pseudomelanosis.
Discussion: Upper GI pseudomelanosis has been linked to various comorbidities, including upper GI bleeding, chronic renal disease, hypertension, and medications such as oral iron, furosemide, hydrochlorothiazide, propranolol, and hydralazine. The present case shows a similar association with iron and furosemide but without the presence of chronic kidney disease, in contrast to all the previously reported cases that suggest a very strong association with iron therapy or chronic renal failure with pseudomelanosis. In addition, women have been reported to have the most cases compared to men. It has been postulated that drug-based sources of sulfur, such as furosemide, disrupt iron transport and cause iron accumulation within macrophages. While the pathogenesis is not clearly understood, no clinical or prognostic significance has been described and no surveillance or follow-up guidelines have been identified. Therefore, it is essential to diagnose patients early on histopathology findings and to avoid unnecessary testing and interventions.

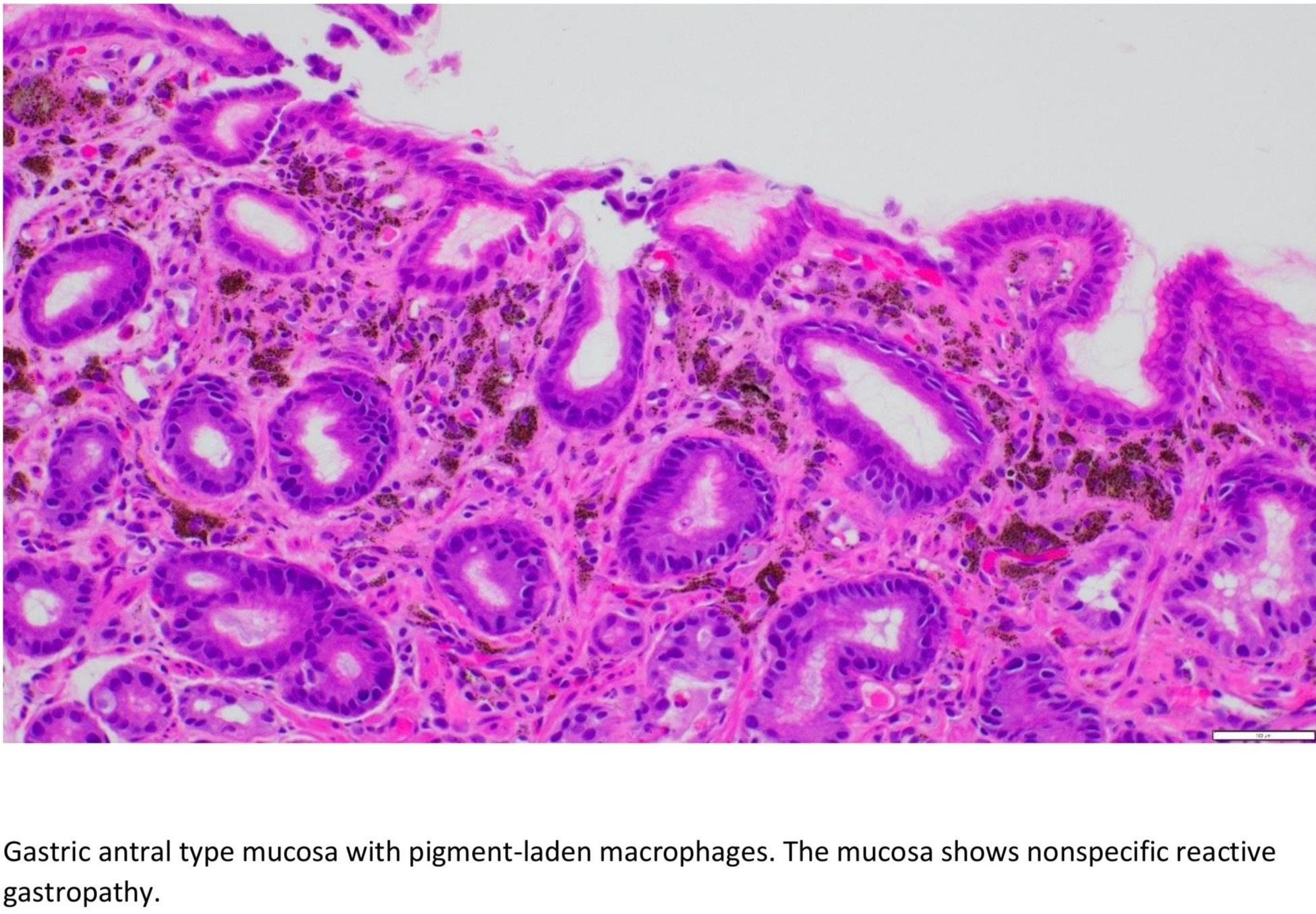
Figure: Gastric antral type mucosa with pigment-laden macrophages. The mucosa shows nonspecific reactive gastropathy.
Disclosures:
Muhammad Usman Shahbaz indicated no relevant financial relationships.
Qasim Manzoor Amjad indicated no relevant financial relationships.
Bilal Khan indicated no relevant financial relationships.
Mariyam Qureshi indicated no relevant financial relationships.
Muhammad Shariq Akram indicated no relevant financial relationships.
Khalil Ur Rehman indicated no relevant financial relationships.
Muhammad Usman Shahbaz, MBBS1, Qasim Manzoor Amjad, MBBS1, Bilal Khan, MBBS1, Mariyam Qureshi, MBBS2, Muhammad Shariq Akram, MBBS2, Khalil Ur Rehman, MBBS2. P1389 - Gastric and Duodenal Pseudomelanosis: A Rare Association with Chronic Iron and Diuretic Therapy, ACG 2023 Annual Scientific Meeting Abstracts. Vancouver, BC, Canada: American College of Gastroenterology.
