Tuesday Poster Session
Category: Liver
P3841 - Do We Really Need CMV Prophylaxis in Every Aviremic High Risk CMV-Seropositive Liver Transplant Recipients (D+/R+) in Pakistani Population
Tuesday, October 24, 2023
10:30 AM - 4:00 PM PT
Location: Exhibit Hall

Azhar Hussain, MD
SUNY Upstate Medical University, New York
Syracuse, New York
Presenting Author(s)
Abdul Wahab Dogar, MBBS, FCPS1, Azhar Hussain, MD2, Kaleem Ullah, MBBS, FCPS1, Shams Ud-Din, MBBS, FCPS1, Abdul Basit Khan, MBBS3, Abdul Ghaffar, MBBS, FCPS1, Abu Hurairah, MD4
1Pir Abdul Qadir Shah Jeelani Institute of Medical Sciences, Gambat, Sindh, Pakistan; 2SUNY Upstate Medical University, New York, Syracuse, NY; 3Nishtar Medical College, Multan, Punjab, Pakistan; 4AdventHealth, Orlando, FL
Introduction: Cytomegalovirus (CMV) infection is a common complication after liver transplantation that can affect graft and patient survival. The aim of this study was to evaluate post-operative outcomes of living donor liver transplant recipients without any post-LDLT cytomegalovirus prophylaxis with ganciclovir or valganciclovir.
Methods: We retrospectively analyzed 358 liver transplant recipients who underwent CMV PCR testing at 7th and 30th postoperative days after transplantation. We did not give any pharmacologic CMV prophylaxis post-LDLT with ganciclovir or valganciclovir. We compared the clinical characteristics and outcomes of the post-op CMV PCR positive group and the negative group and did a literature review while comparing our immediate and longterm post-LDLT outcomes with published literature. .
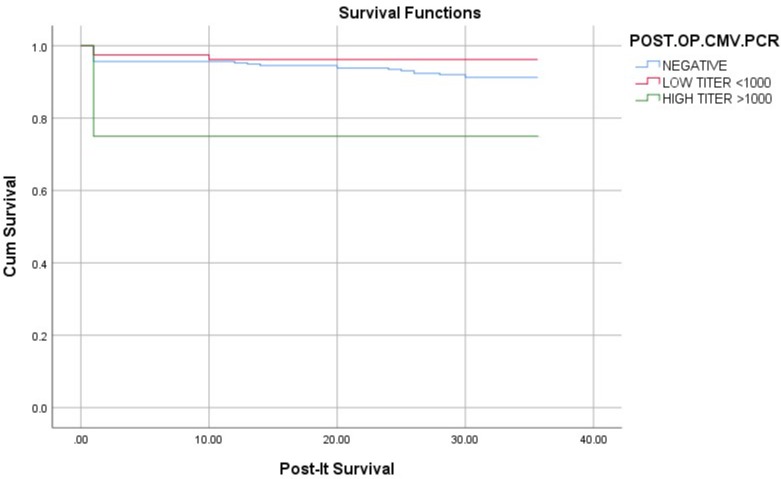
Results: Among 358 liver transplant recipients, 83(23.2%) had positive post-op CMV PCR [low titer (< 1000 IU/mL)=79 & high titer (≥1000 IU/mL)=4]. None of the recipients with low titer positive post-op CMV PCR were treated for active CMV disease. There was no significant difference in the survival time among the post-op CMV PCR groups (log-rank test p=0.143). However, the post-op CMV PCR positive group had a higher incidence of acute rejection episodes than the negative group (18.2% vs 7.1%, p=0.028). The post-op CMV PCR positive group also had a lower estimated glomerular filtration rate (eGFR) at 12 months than the negative group (54.6 ± 19.4 vs 63.4 ± 18.7 ml/min/1.73m2, p=0.046).
Discussion: In this retrospective cohort study, 358 liver transplant recipients were followed for 3 years post-LDLT. 83(23.2%) had positive post-op CMV PCR [low titer (< 1000 IU/mL)=79 & high titer (≥1000 IU/mL)=4]. We did not treated any of the recipients with low titer positive post-op CMV PCR for active CMV disease and were observed with serial LFTs, RFTs and clinically. There was no difference in post-LDLT survival outcomes between different study groups. Also, Post-operative CMV PCR positivity and lack of post-operative CMV prophylaxis were associated with increased risk of acute rejection and impaired graft function in living donor liver transplant recipients. Early detection and treatment of CMV infection may improve liver transplant outcomes.
Disclosures:
Abdul Wahab Dogar, MBBS, FCPS1, Azhar Hussain, MD2, Kaleem Ullah, MBBS, FCPS1, Shams Ud-Din, MBBS, FCPS1, Abdul Basit Khan, MBBS3, Abdul Ghaffar, MBBS, FCPS1, Abu Hurairah, MD4. P3841 - Do We Really Need CMV Prophylaxis in Every Aviremic High Risk CMV-Seropositive Liver Transplant Recipients (D+/R+) in Pakistani Population, ACG 2023 Annual Scientific Meeting Abstracts. Vancouver, BC, Canada: American College of Gastroenterology.
1Pir Abdul Qadir Shah Jeelani Institute of Medical Sciences, Gambat, Sindh, Pakistan; 2SUNY Upstate Medical University, New York, Syracuse, NY; 3Nishtar Medical College, Multan, Punjab, Pakistan; 4AdventHealth, Orlando, FL
Introduction: Cytomegalovirus (CMV) infection is a common complication after liver transplantation that can affect graft and patient survival. The aim of this study was to evaluate post-operative outcomes of living donor liver transplant recipients without any post-LDLT cytomegalovirus prophylaxis with ganciclovir or valganciclovir.
Methods: We retrospectively analyzed 358 liver transplant recipients who underwent CMV PCR testing at 7th and 30th postoperative days after transplantation. We did not give any pharmacologic CMV prophylaxis post-LDLT with ganciclovir or valganciclovir. We compared the clinical characteristics and outcomes of the post-op CMV PCR positive group and the negative group and did a literature review while comparing our immediate and longterm post-LDLT outcomes with published literature. .
Results: Among 358 liver transplant recipients, 83(23.2%) had positive post-op CMV PCR [low titer (< 1000 IU/mL)=79 & high titer (≥1000 IU/mL)=4]. None of the recipients with low titer positive post-op CMV PCR were treated for active CMV disease. There was no significant difference in the survival time among the post-op CMV PCR groups (log-rank test p=0.143). However, the post-op CMV PCR positive group had a higher incidence of acute rejection episodes than the negative group (18.2% vs 7.1%, p=0.028). The post-op CMV PCR positive group also had a lower estimated glomerular filtration rate (eGFR) at 12 months than the negative group (54.6 ± 19.4 vs 63.4 ± 18.7 ml/min/1.73m2, p=0.046).
Discussion: In this retrospective cohort study, 358 liver transplant recipients were followed for 3 years post-LDLT. 83(23.2%) had positive post-op CMV PCR [low titer (< 1000 IU/mL)=79 & high titer (≥1000 IU/mL)=4]. We did not treated any of the recipients with low titer positive post-op CMV PCR for active CMV disease and were observed with serial LFTs, RFTs and clinically. There was no difference in post-LDLT survival outcomes between different study groups. Also, Post-operative CMV PCR positivity and lack of post-operative CMV prophylaxis were associated with increased risk of acute rejection and impaired graft function in living donor liver transplant recipients. Early detection and treatment of CMV infection may improve liver transplant outcomes.

Figure: Kaplan-Miere survival curve showing 40 months post-LDLT survival outcomes in different study groups (log-rank- Mantel-Cox p=0.41)
Disclosures:
Abdul Wahab Dogar indicated no relevant financial relationships.
Azhar Hussain indicated no relevant financial relationships.
Kaleem Ullah indicated no relevant financial relationships.
Shams Ud-Din indicated no relevant financial relationships.
Abdul Basit Khan indicated no relevant financial relationships.
Abdul Ghaffar indicated no relevant financial relationships.
Abu Hurairah indicated no relevant financial relationships.
Abdul Wahab Dogar, MBBS, FCPS1, Azhar Hussain, MD2, Kaleem Ullah, MBBS, FCPS1, Shams Ud-Din, MBBS, FCPS1, Abdul Basit Khan, MBBS3, Abdul Ghaffar, MBBS, FCPS1, Abu Hurairah, MD4. P3841 - Do We Really Need CMV Prophylaxis in Every Aviremic High Risk CMV-Seropositive Liver Transplant Recipients (D+/R+) in Pakistani Population, ACG 2023 Annual Scientific Meeting Abstracts. Vancouver, BC, Canada: American College of Gastroenterology.
